Edema& LEG VEIN / DVT
Vein Specialist

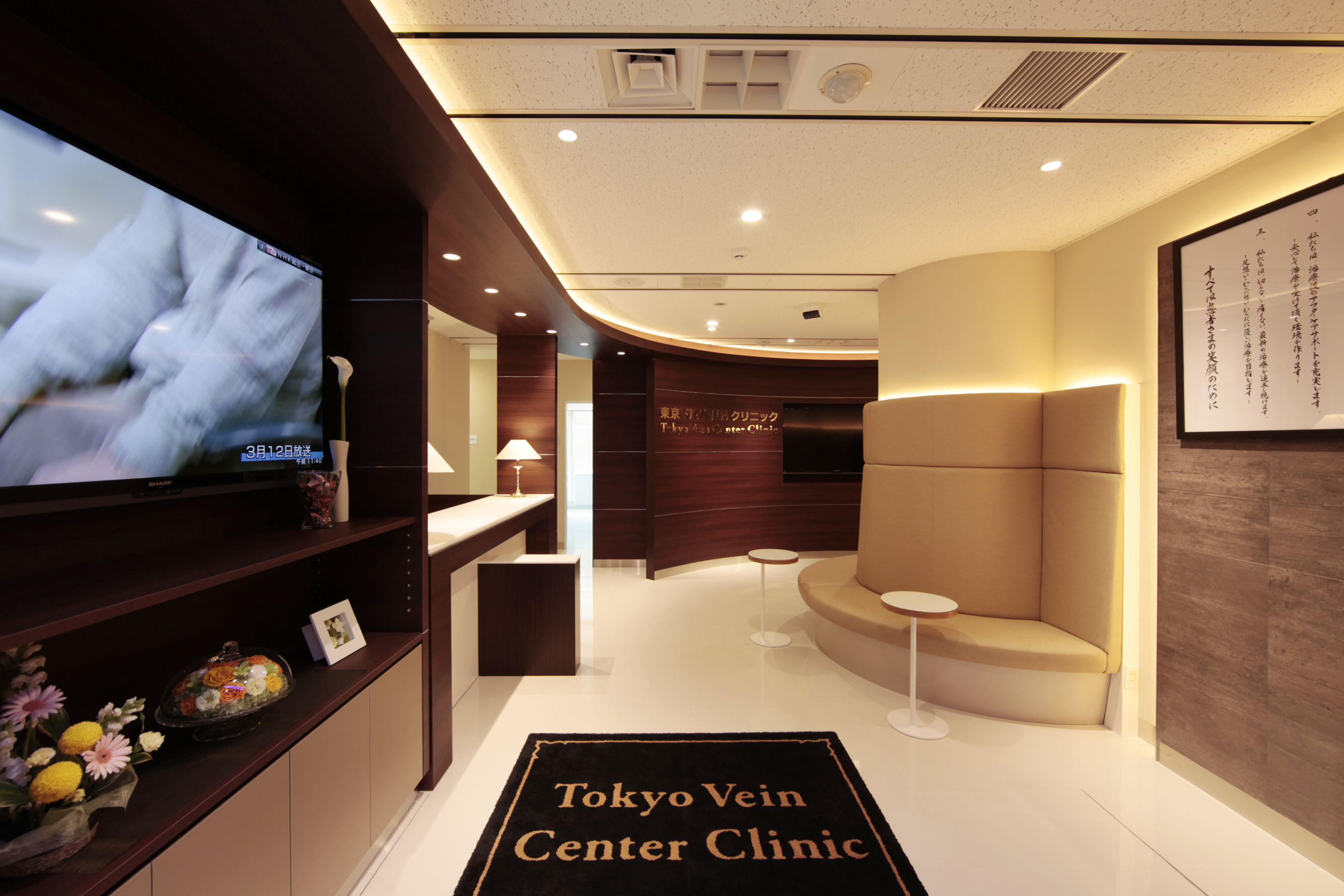
Our hospital was established in 2006 in Chiyoda-ku, Tokyo as a specialized hospital for vascular diseases such as lower limb varicose veins. We offer “prevention,” “examination,” and “treatment.” In addition, we are able to provide “advanced treatment” in collaboration with university hospitals and affiliated hospitals, “standard treatment under insurance coverage (insured group treatment),” and “second opinions.” Please contact us first by phone or email.
Diagnosis is most important. The patient is the main character. Correct diagnosis is the most important thing in order to correctly understand a disease. Therefore, first of all, we listen in detail to the patient’s symptoms, lifestyle, and stories. Then, we perform a detailed diagnosis with ultrasound (echo) exams of the abdomen and legs, as well as blood and urine tests. We then select the most appropriate treatment method together, including the patient’s wishes, based on a comprehensive analysis of all of these factors. Our hospital provides medical advice on the best treatment method based on the patient’s condition, but the patient always makes the final decision on the treatment method. We also have a patient support room staffed by professionals who provide individualized support.
Clinic Hours 10:00 AM to 1:00 PM and 3:00 PM to 7:00 PM (Closed on Thursday and Sunday)
Reservations by Phone, Email, or LINE We accept reservations by phone or email. Feel free to contact us by phone or email with any concerns, such as “My feet feel weak,” “Veins are becoming visible,” “My feet hurt,” “My feet are numb,” and more. The “Patient Support Room” will respond.
Note: As of January 2023, we do not respond to inquiries regarding post-corona syndrome or keloid scars by phone.
Free email consultation is available 24 hours a day, 365 days a year. Please feel free to consult us. It will be handled by the “Support Room”.
Note: We have been receiving a lot of wrong number calls lately. Please be careful not to make a mistake when making a call. Note: To accurately understand the contents of the calls we receive from customers, we record them.
DVT
Deep vein thrombosis is the formation of blood clots (thrombi) in the deep veins, usually in the legs.
Blood clots may form in veins if the vein is injured, a disorder causes the blood to clot, or something slows the return of blood to the heart.
Blood clots may cause the leg or arm to swell.
A blood clot can break loose and travel to the lungs, which is called a pulmonary embolism.
Doppler ultrasonography and blood tests are used to detect deep vein thrombosis.
Anticoagulants are given to prevent clot enlargement and prevent pulmonary embolism.
There are two main types of veins, superficial and deep. Superficial veins are located in the fatty layer under the skin. Deep veins are located in the muscles and along the bones.
Spider vein
LEG VEIN
The leg veins are blood vessels that carry blood from the legs back to the heart. They play a crucial role in the circulatory system and are responsible for returning blood to the heart for re-oxygenation.
There are two main types of leg veins: superficial veins and deep veins. Superficial veins are located just below the surface of the skin and can be easily seen, while deep veins are located deeper within the leg and are not visible from the surface.
Varicose veins are a common problem that can affect the legs. They occur when the veins become enlarged, swollen, and twisted, and can cause a range of symptoms including pain, swelling, and aching in the legs. In some cases, varicose veins can also lead to more serious complications such as blood clots.
If you are concerned about your leg veins, it is important to seek the advice of a doctor or specialist. They can perform a number of tests to determine the cause of your symptoms and recommend the most appropriate treatment. In some cases, this may involve lifestyle changes, such as exercise and weight management, while in other cases, it may involve more invasive treatments such as surgery or vein ablation.
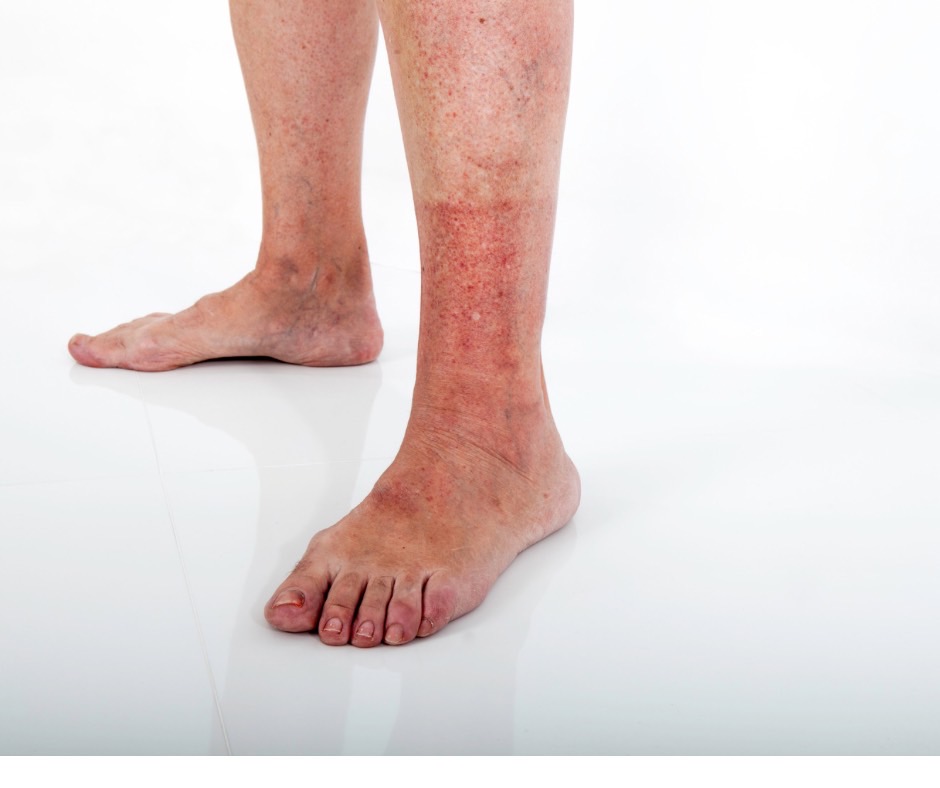
Lower Limb Edema
So far, our clinic has provided treatment for varicose veins and instructed the use of compression stockings to many patients through our lower limb edema outpatient department. However, despite the fact that surgery alone may not be enough to cure it, there has been an increase in patients who are left untreated. This has become even more difficult during the COVID-19 pandemic, as it is hard for people to go to medical facilities and they often come to us after their condition has worsened.
That is why our clinic has established a new “Lower Limb Edema-related Diseases Outpatient Department” that goes beyond just treating edema.
Are you currently facing such a situation?
Please contact us by LINE or e-mail
Case1
Have you undergone surgery for varicose veins but still experience edema, with no effective solution provided by medical facilities despite seeking their advice?
Or have you been prescribed compression stockings despite no abnormalities being found through a lower limb vein echo, and despite your best efforts, your legs still hurt in the evening and you end up taking them off?
This is no longer just a problem with varicose veins, there may be possibilities of health issues related to lifestyle or internal organs. Therefore, without accurate diagnosis and treatment, it will not heal.
Case 2
Have you undergone surgery for varicose veins but still experience edema, with no effective solution provided by medical facilities despite seeking their advice?
Or have you been prescribed compression stockings despite no abnormalities being found through a lower limb vein echo, and despite your best efforts, your legs still hurt in the evening and you end up taking them off?
This is no longer just a problem with varicose veins, there may be possibilities of health issues related to lifestyle or internal organs. Therefore, without accurate diagnosis and treatment, it will not heal.
Case 3
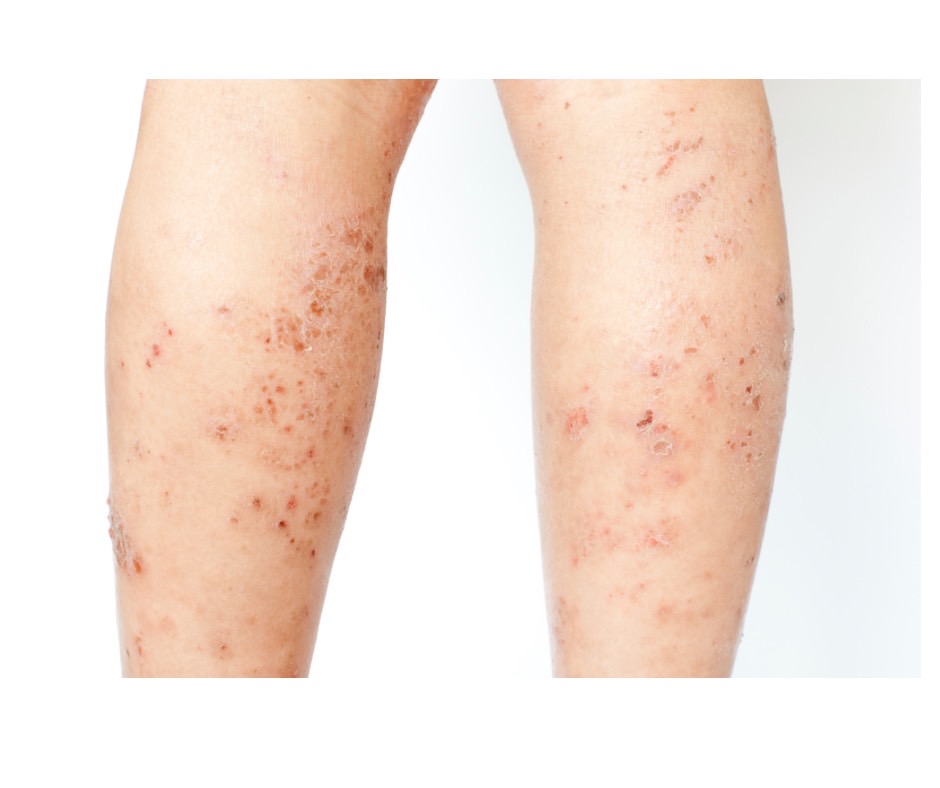
Are there those among you who have net-like veins appearing on the skin but are unable to receive any treatment as no abnormalities were found through a lower limb vein echo?
This is not varicose veins but rather telangiectasia. This can also be due to pigmentation deposition caused by inflammation of the tiny blood vessels responsible for microcirculation in the skin, which can occur as a symptom of skin vasculitis, one of the conditions that can occur with exposure to heat sources such as stoves and fireplaces, or in the case of autoimmune diseases or allergies. In this case, treatment for ordinary pigmentation deposition or for varicose veins will not heal the condition.
Cellulitis
What is cellulitis?
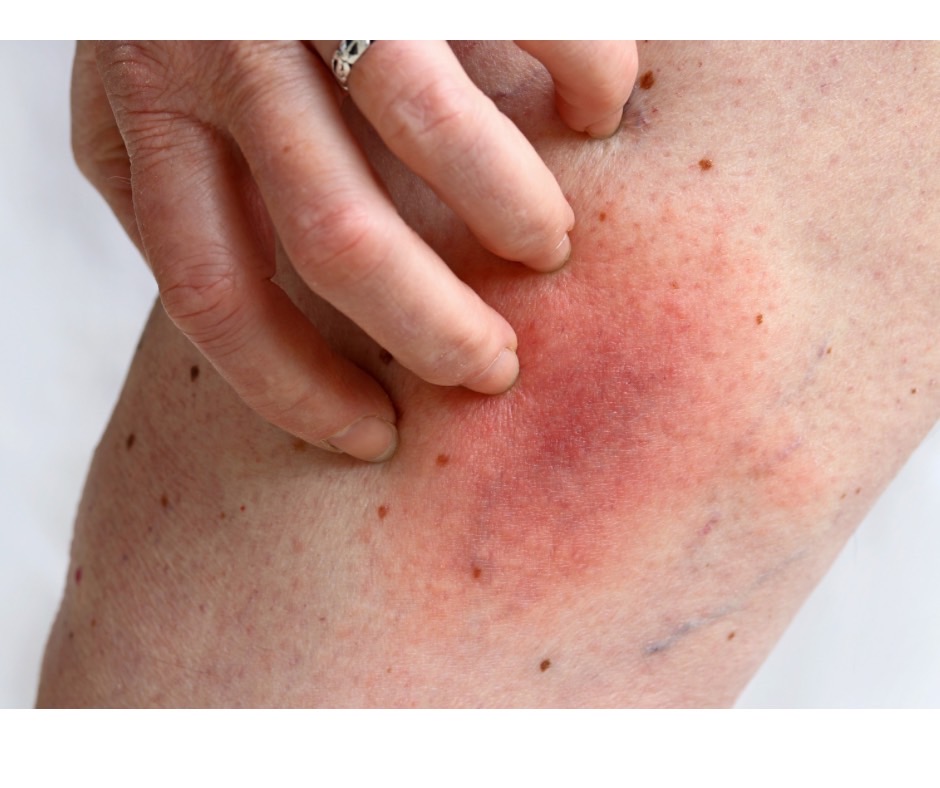
Cellulitis is a bacterial skin infection that affects the skin and the subcutaneous tissue immediately beneath it. It is also called “hives”.
Symptoms include redness, swelling, heat, and pain in the affected skin area, which can rapidly spread. In some cases, there may also be symptoms such as fever, chills, and fatigue. Cellulitis is common in the shins or toes, but it can also occur in other parts of the body. Usually, it does not occur in multiple areas simultaneously.
The human skin is protected from the easy invasion of bacteria and foreign objects, but if bacteria that entered through cuts, scratches, insect bites or after surgery reach the subcutaneous tissue, it causes cellulitis. Even if there are no such injuries, factors that lower immunity, such as diabetes or steroid treatment, can cause cellulitis to become severe.
In addition, interstitial fluid (moisture accumulated between cells) in the swollen area contains a lot of protein, fat, and waste such as broken cells and bacteria, and is an environment where bacteria can easily multiply. People with swelling in their legs due to lymphatic swelling are more prone to cellulitis.
Treatment:
Since cellulitis is a symptom caused by bacterial infection, treatment involves antibiotics. Symptoms usually improve within a week. If there is still inflammation or fever, treatment may need to be changed from oral to intravenous. If there is pain or fever, medication to relieve symptoms may also be prescribed.
In addition to treatment with antibiotics, rest and elevation of the affected area and cooling can help relieve symptoms and speed up recovery. If there is an abscess in the affected area, drainage may be necessary.
Prevention:
As stated above, cellulitis is caused by bacteria entering the skin, so it is important to keep the skin clean and maintain barrier function to prevent bacteria from entering the body. Of course, basic measures such as hand washing and gargling are important, and if a wound is made, it is important to properly clean the wound with soap, etc., and to moisturize after bathing or doing water-based work.
Stasis Dermatitis
What is Stasis Dermatitis?
Stasis dermatitis is similar to cellulitis and is characterized by red, swollen skin with tenderness, which originates from deep within the fat tissue under the skin. Unlike cellulitis, which is caused by bacteria, stasis dermatitis is caused by venous insufficiency, which is a condition in which blood does not properly flow back to the heart.
Cause
Normally, blood flows towards the heart, but when blood flow is slowed down due to long periods of standing, desk work, lack of exercise, illness or other causes, water accumulates in the blood. The increased pressure in the vessels leads to fluid (interstitial fluid) being pushed out of the vessels and into the surrounding tissue. This fluid is not easily reabsorbed back into the veins and if it remains unabsorbed for a prolonged period, it can cause the soft skin to break down, resulting in a firm and less elastic skin. The pressure between this hard skin and the surrounding fat tissue causes inflammation and symptoms such as pain and redness.
Many patients come to the clinic with complaints such as “I can’t seem to get rid of the swelling, but now the pain and redness are getting stronger”.
Treatment and Prevention
To improve the state where excessive water accumulates in the vessels, it is necessary to use elastic stockings or elastic bandages to apply pressure from the outside, to improve the living habits such as doing physical activity in the legs during standing work, and to reduce weight. For patients with excessive fluid, water control is carried out with diuretics or herbal medicine.
If the cause of the venous insufficiency is varicose veins in the legs, treatment…
Vasculitis
What is Vasculitis
Do you have red or purple spots on your skin or noticeable blood vessel color that you are concerned about? Some people may also have accompanying symptoms such as itching, feeling hot or cold, or tingling sensations. These may be caused by a disease called “vasculitis,” which is inflammation of the blood vessels.
Vasculitis refers to a disease that is caused by inflammation of the blood vessels themselves. The causes can include abnormal self-immune response, infection with microorganisms, or medication. Blood vessels are spread throughout the entire body from head to toe, so there is a possibility that symptoms will appear in various organs throughout the body.
Among them, the skin is a frequent site of onset, and vasculitis that occurs in the skin is called “cutaneous vasculitis.” The most common area of onset is the lower legs.
Symptoms
In cases where symptoms occur throughout the body, in addition to skin symptoms such as red spots appearing on the skin or blood vessels appearing to spread like a net, there may also be systemic symptoms such as fever, general fatigue, loss of appetite, weight loss, muscle and joint pain, etc. Symptoms may also appear in organs such as the lungs, digestive system, and kidneys.
The skin consists of the epidermis, dermis, and subcutaneous tissue.
By doing a skin biopsy, you can determine whether the lesion is occurring in the vessels of the dermis, at the boundary between the lower layer of adipose tissue, whether it is occurring in veins or arteries.
Team medicine
Team medicine As described above, skin lesions can be caused by more than just congestion, and a wide perspective is needed when making a diagnosis. Our clinic approaches your symptoms by using knowledge that spans across three fields: vascular surgery, plastic surgery, and dermatology, and our “team of specialist doctors for the feet” will work together to diagnose and treat your condition.
We also refer patients to the “Foot Disease Center” at Juntendo University (located in Tokyo’s Bunkyo ward) as needed.